Despite their numerous health advantages, all sports run the risk of overusing certain parts of the body, resulting in injuries. Due to their close contact nature, contact sports are notoriously high risk activities when it comes to injuries. Grappling arts, that involve or focus on controlling the opponent by grabs and weight tend to show a regular pattern of damage. To receive the right care and assist in the recovery process, it is crucial to have basic knowledge about the attention these injuries require, as inadequate healing can lead to recurring or snowballing effect.
While in contact sports like rugby, players are usually prone to suffer trauma and concussions, which can threaten with brain damage, in grappling arts practitioners tend to injure their joints. When fighters grab their opponents and lock them in certain positions, they often cause an abnormal rotation of the joint. The purpose of this article is to provide a summary of the most common injuries that occur in contact sports, with a particular emphasis on grappling arts.
Muscle strains
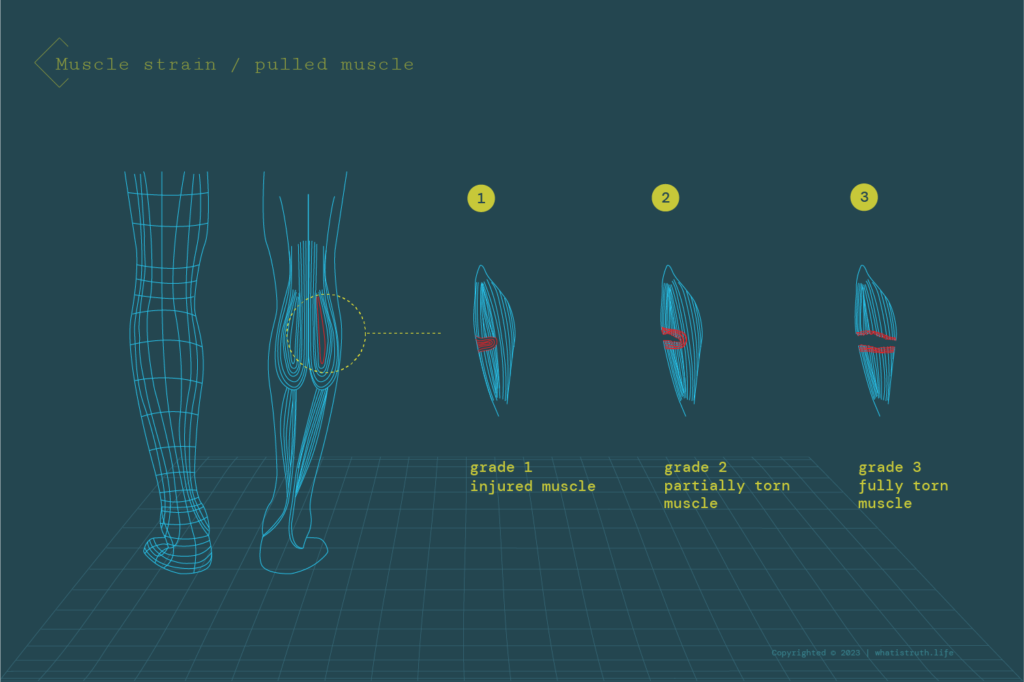
A muscle strain, also known as a pulled muscle, is a common injury that can happen to any muscle. This occurs when the targeted muscle is stretched beyond its limit as a consequence of putting the muscle fibres under too much stress. In certain instances, this injury can result in a partial or complete muscle tear. May occur immediately as a result, for example, of a direct hit during training, coming with immediate pain. But it can also develop over time as a result of repetitive movement regularly overstretches the muscle, resulting in the muscle or tendon slowly becoming weak.
In certain instances, the strain can affect the tendon that connects the muscle to the bone. Muscle strains are classified into grade 1, grade 2, and grade 3, the former being the most frequent, while in case of grade 3 muscle strains the injury might require surgery to reattach the muscle.
Potential causes:
- Muscle tightness due to inadequate warm up before exercising
- Attempting to do too much, too quickly during exercise
- Direct hit on the muscle
- Regular overuse of the muscles
Usual symptoms:
- Swelling of the area
- Pain
- Tenderness
- Bruising
- Muscle spasms and weakness
Suggested treatment
For lower grade strains it is common to improve with home treatment alone without any medical intervention. The standard protocol to treat the strain after the injury is known as the R.I.C.E (Rest, Ice, Compression, Elevation) method.
- Rest: Resting the muscle is the first step to take. Avoid any physical activity or movement that uses that muscle and causes pain or discomfort in the following days.
- Ice: Applying cold therapy right after an injury can help reduce swelling and pain. It is recommended to apply an ice pack to the affected muscle for 15-20 minutes every 2-3 hours. Wrap the icepack into cloths if it hurts your skin.
- Compression: Lightly wrap the injured area using compressive bandages. This also decreases swelling and stabilizes the body part. However, these bandages should not be too tight to prevent appropriate blood flow to the region.
- Elevation: Elevating the injured body part can lower the blood flow into it and reduce swelling.
Over-the-counter pain killers and non-steroidal anti-inflammatory medication can also be used to reduce pain and swelling. Special exercises can be provided by physiotherapists or online physio practices to assist in recovering. After the acute stage, sports massage can help eliminate scar tissue and keep the muscle flexible. Scar tissue can trap the nerves and cause pain. Proper recovery and caution is essential, as an injured muscle is highly susceptible to reinjury.
Knee sprains
The knee is the most commonly injured part of the lower body in grappling arts. A knee sprain is an injury that affects the ligaments that stabilize your joint and connect the bones. The injury is usually accompanied by a popping sound and can cause the leg to buckle when you try to stand on it. The following 1-2 days may bring on swelling and typically severe pain.
The knee is a relatively complex structure, with 4 ligaments and multiple muscles that are entangled with nerves. The Anterior Cruciate Ligament (ACL) is the most frequently affected one, followed by the Medial Collateral Ligament (MCL). In contact sports, the most commonly injured ligament is the ACL due to the sudden stop or change of direction while attacking or passing guard. Grapplers can also injure their ACLs during leg locks when the joint is bent at unnatural angles.
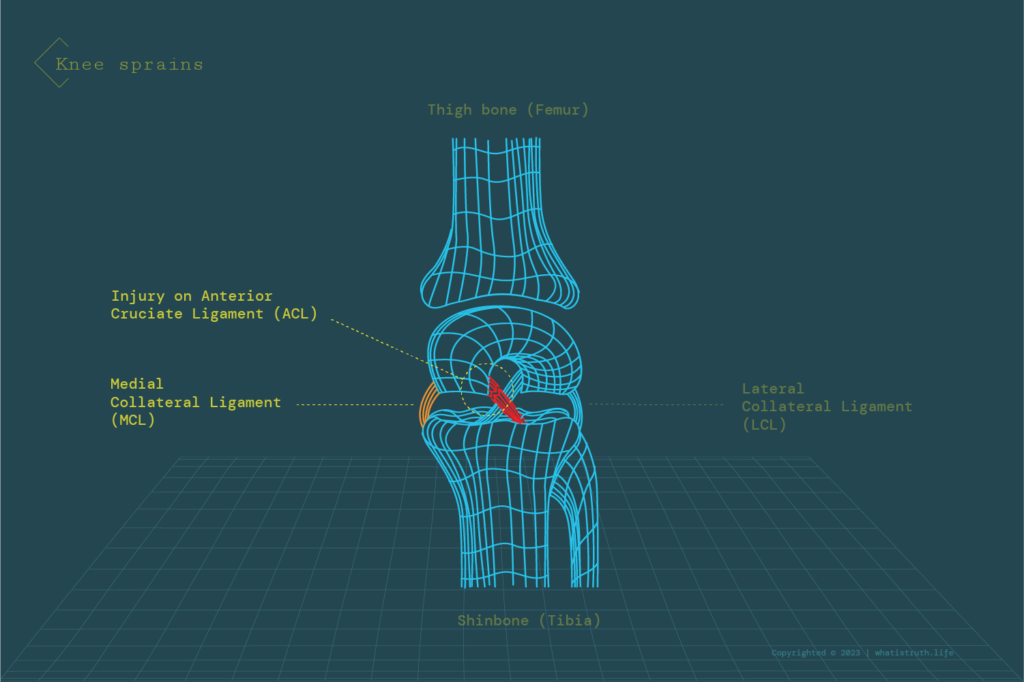
Knee sprains can also be categorised into 3 grades, where grade 1 is a mild injury with stretched ligament, grade 2 involves a partial tear, and grade 3 involves a complete rupture of the ligament.
Usual symptoms:
- Severe pain
- Swelling or bruising
- Limited knee range of motion
- Popping sensation in the knee
- Instability
- Knee looks deformed
Suggested treatment
It is recommended to use the earlier described R.I.C.E method for first aid immediately after an injury in order to prevent it from getting worse. Over-the-counter painkillers and non-steroidal anti-inflammatory drugs can be added when the swelling appears (usually after 1-2 days).
However, if no improvement occurs within two weeks, you should seek medical attention for the correct diagnosis and treatment plan. In this case, the severity of the tear and the exact ligament or potentially damaged other tissues require a detailed examination and/or scanning. Based on the result, the doctor can suggest rehabilitation which can commence once the swelling and bruising have been reduced, typically with the assistance of a specialized physiotherapist or online knee exercise program. The received injury-specific exercises help to restore the knee’s range of motion.
Severe cases, like grade 3 injuries, however, might require surgical intervention, especially in case of professional athletes where gaining back the full range of motion is essential to continue with their career.
Meniscal Injury
The meniscus is a cartilage in the knee that acts as a pillow between the bones. It’s quite prone to tearing in contact sports. Usually caused by jumping, especially with speed and weight, like during guard pass and takedown in grappling training. But meniscus injury also can occur during any activity that involves forcefully twisting or rotating your knee, particularly with full weight on it.

Usual symptoms:
- Medium or severe knee pain, especially in twisting or rotating motions
- Swelling or stiffness
- Knee locking in position
- Difficulty to bend or fully extend the knee
Suggested treatment
The R.I.C.E method mentioned earlier is the initial treatment for the injury. The swelling can take 24 hours to appear, taking medication before that is not recommended. Medical treatment is only necessary if the symptoms don’t improve within 1-2 weeks. After it worth to visit a doctor for psychotherapy recommendations. In many cases, physiotherapy is sufficient to reduce stress on the knee, increase range of motion, and strengthen the muscles to protect the area.
However, the self-healing capacity of the cartilage is very limited because it lacks own blood supply. If the tear is severe or there is a broken piece of the meniscus causing other potential problems, surgery may be required.
Swollen knee cap (Prepatellar bursitis)
Prepatellar bursitis is a condition, often called as housemaid’s knee, that can happen when the knee receives constant direct impacts on the knee cap from regular kneeling or falling on the floor. The bursa, that gets swollen, is a small sac filled with fluids that acts as a protective cushion for your joint. Regular irritation of the bursa causes it to swell and the extra fluid produced puts pressure on other parts of the knee.

Usual symptoms:
- Noticeable knee swelling, deformed looking knee
- Limited range of motion
- Pain (not always)
Suggested treatment
Patella’s bursitis is usually a minor injury and disappears with enough rest. Over-the-counter non-steroidal anti-inflammatory drugs may contribute to reducing swelling and discomfort. If the swelling persists after using the usual R.I.C.E. method for one or two weeks, the doctor may recommend corticosteroid injections.
Fever and red colouring in the swelling area indicate a bacterial infection, likely due to an open wound in the knee. This requires immediate medical treatment and it’s highly recommended that you visit the nearest emergency department or hospital in this case.
Ankle sprain
Ankle sprains are another common injury among wrestlers and grapplers. Similarly to knee sprain, it also affects the ligaments that hold the ankle bones together. The injury has similar symptoms to a knee sprain, including swelling and limited range of motion. This type of injury usually results from twisting the ankle in abnormal positions, planting the foot the wrong way during a fight, or stepping on the opponent and losing balance.
Suggested treatment
Just as with a knee sprain, the first aid treatment would be the R.I.C.E method. After the swelling reduced, physiotherapy can be utilized to improve the ankle condition and help to regain its strength and complete range of motion.
If the ankle does not improve within 1-2 weeks, you need to see a doctor. The doctor could suggest using crutches and bandages to avoid tension in the ankle. In severe cases, a cast may be applied to the ankle to immobilize it while the ligament heals. Only after the restriction removed, a specific physiotherapy or online ankle exercise program can start to build back the muscles and improve mobility.
Surgery also can be a viable treatment option in severe cases, particularly for professional athletes who likely will place the ankle under further pressure.
Shoulder and elbow dislocations
When a bone pops out of its socket, it is referred to as a dislocation. In grappling arts, such as wrestling, BJJ, or combative arts with grappling components, such as mixed martial arts, shoulders and elbows have just as high dislocation risk as the finger have.
Dislocation can happen due to the severe pressure these joints are placed under when doing different manoeuvres or falling. Depending on its severity, dislocation can also injure the tendon, ligaments, nerves, blood vessels, and muscles around the joint at the same time which can increase the pain and cause a numbness or tingling sensation in the surrounding area.
Potential causes:
- Extreme twisting of the shoulder or elbow joint
- Forced pull or sudden hit on the joint
- Falling on the joint with the body weight
Usual symptoms:
- Severe pain
- Out-of-place shoulder or elbow with visible deformity
- Inability to move the joint
- Swelling or bruising
- Numbness or tingling
Suggested treatment
It is necessary to seek immediate medical attention after a dislocation. To prevent any further injury while waiting for treatment, put ice on the area to reduce swelling and if possible, use a splint to immobilize the joint. Since the joint can dislocate to several direction and into different degree, affecting the surrounding tissues, it can only be repositioned by a trained professional. Attempting to do it without proper training can result in more damage to your joint and tissues. In case of inflammation the doctor might administer cortisone injection as well. In severe cases, surgery might be needed to repair the joint and the tissues involved.
After the joint has been repositioned, it must be immobilized for a few days and only after the swelling decreased, the physiotherapy or online shoulder exercise program can start to strengthen the muscles to prevent future dislocation. The exercises are usually performed for 8 to 10 weeks following dislocation. It is essential to avoid putting pressure on the shoulder or elbow in the recovery period, which can take several months. When the shoulder is dislocated, the joint can be subject to repeated dislocations, so increased awareness is required during training.
Cauliflower ear
The cauliflower ear, also known as a subperichondrial hematoma, is a common injury among wrestlers, giving practitioners a distinctive appearance.
It occurs when the ear suffers a heavy trauma, usually pressed to the ground or being folded during training. The pressure causes a blood pocket to form under the skin. As it gets bigger, the ear folds in on itself, causing a noticeable deformity and in severe cases, a decrease in hearing.
Usual symptoms:
- Pain
- Hearing loss
- Ear deformity
- Swelling or bruising
Suggested treatment
This condition can only be treated by a doctor. The procedure involves making a small incision in the ear to drain the blood. To prevent permanent deformities, it is recommended to seek medical attention within 6 hours of the injury.
References
Andrews, K., Lu, A., Mckean, L., & Ebraheim, N. (2017). Review: Medial collateral ligament injuries. Journal of Orthopaedics, 14(4), 550–554. https://doi.org/10.1016/j.jor.2017.07.017
Błach, W., Smolders, P., Rydzik, Ł., Bikos, G., Maffulli, N., Malliaropoulos, N., Jagiełło, W., Maćkała, K., & Ambroży, T. (2021). Judo injuries frequency in Europe’s top-level competitions in the period 2005–2020. Journal of Clinical Medicine, 10(4), 852. https://doi.org/10.3390/jcm10040852
Dislocated shoulder: Causes, treatment & prevention. Cleveland Clinic. (2023, May 11). https://my.clevelandclinic.org/health/diseases/17746-dislocated-shoulder
Hinz, M., Kleim, B. D., Berthold, D. P., Geyer, S., Lambert, C., Imhoff, A. B., & Mehl, J. (2021). Injury patterns, risk factors, and return to sport in Brazilian Jiu Jitsu: A cross-sectional survey of 1140 athletes. Orthopaedic Journal of Sports Medicine, 9(12), 232596712110625. https://doi.org/10.1177/23259671211062568
Mayo Clinic Staff . (2022, December 1). ACL injury. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/acl-injury/symptoms-causes/syc-20350738
Mayo Clinic Staff. (2022, August 11). Sprained ankle. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/sprained-ankle/symptoms-causes/syc-20353225
Mayo Clinic. (2022, October 11). Muscle strains. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/muscle-strains/diagnosis-treatment/drc-20450520
Patel, B., Skidmore, K., Hutchison, J., & Hatcher, J. (2023, January). Cauliflower ear. National Center for Biotechnology Information. https://pubmed.ncbi.nlm.nih.gov/29261905/
Pietrangelo, A. (2023, April 15). Muscle strains: Symptoms, causes, and prevention. Healthline. https://www.healthline.com/health/strains#_noHeaderPrefixedContent
Rishor, C., & Pozun, A. (2022, September 6). Prepatellar bursitis – statpearls – NCBI bookshelf. National Library of Medicine. https://www.ncbi.nlm.nih.gov/books/NBK557508/
Wheeler, T. (2022, January 26). Meniscus tear in knee: Symptoms, causes, and treatments. WebMD. https://www.webmd.com/pain-management/knee-pain/meniscus-tear-injury



